Exercises for lower back pain is a critical and non-negotiable part of treatment and rehabilitation. This is about as close to an agreed upon, universal, undisputed fact that we can get when it comes to musculoskeletal care. And this applies across the spectrum of back pain. Whether the pain is acute, chronic, recurrent, mechanical, neurogenic, or has strong social, psychological, or cognitive-emotional drivers, movement and exercise is a necessary and powerful driver of change and adaptation.
But what exercises are best?
Of course this is a complicated question that involves many factors. It’s not just the type of back pain that must be considered. Variables like frequency, volume, and intensity also need to be taken into account.
We will get to all of these critical factors in the articles that follow. But for now let’s focus on the exercises and movements themselves.
The problem with traditional lower back pain exercises
Most lower back exercise programs are centered around trying to create a more “stable” spine. This line of thinking often equates stability to preventing motion. The thought here is that excessive or unwanted movement of the spinal joints is thought to cause tissue damage and injury. So exercises are prescribed to strengthen the “core”. To build strength or endurance of the muscles surrounding the lumbar spine.
Here we see exercises like planks, side-planks, bird-dogs, and bridges as the primary staple in so many rehab plans. Throw in some abdominal hollowing, or maybe some bracing, and now we’re on our way to a better back.
But there are several problems with this approach.
First, this line of thinking assumes there is an idealized alignment of the spine and too much deviation outside of this posture is unsafe. So these traditional isomeric-based exercises aim to train the spine in a static, ideal, neutral position. Here the belief is that if the spine muscles get stronger they will be able to hold and maintain these “safer” postures during movement and activity.
But just because we train and strengthen the muscles and spine in one specific position does not mean the body will start to somehow adopt and utilize these postures with real-world activities. Movement is far more complicated than that.
And remember the back is supposed to move and contribute to body motion and positioning. That is why the spine evolved as a moveable column and not a single rigid bony segment. Attempting to train static, rigid, idealized positions is not only less effective, but goes against the intended function of the spine.
Specific Adaptation to Imposed Demands
Your body responds to the demands placed upon it. This is the S.A.I.D. principle (Specific Adaptation to Imposed Demands). So if we are training the lower back in a narrow range as outlined above the muscles will adapt and get stronger in that specific posture. But these strength and endurance gains won’t necessarily carry over to other positions. They are only specific to the trained postures.
But what happens when we find ourselves outside of that narrow range?
In this scenario the body will be less prepared to deal with or tolerate these positions. This is the more likely scenario to cause injury. It’s not so much that too much flexion or extension is bad. It’s that the body is less capable of controlling the spine and tolerating the stresses associated with these untrained positions. Instead of training the spine to avoid these “dangerous” postures perhaps a better and more realistic approach is to train the spine to control and better tolerate these positions?
It’s About Control. Which Means It’s About the Nervous System
The use of these isometric-based exercises also assumes stability to be primarily related to muscle strength or endurance. But this is really a poor understanding of what stability is. Stability is really not so much about strength and endurance as much as it is about the ability to control the joints.
Remember the spine is going to move. It needs to. It’s supposed to. What’s most important is for each of these spinal joints to be controlled throughout the range of movements they perform. And this control is really more about the nervous system.
But traditional isometric-based “core” exercises place little to no demand on the nervous system. At least not from a joint control perspective. There is contraction and force-production demand but no movement demand. So there is minimal communication between the sensory and motor systems. There is no need for the CNS to adjust muscle tension which is needed to produce and control joint motion.
Remember the S.A.I.D. principle. If we are not performing exercises that tap into and challenge nervous system control this aspect of muscle coordinationl and stability will not improve and adapt.
Stability is really not so much about strength and endurance as much as it is about the ability to control the joints.
Use It Or Lose It
We know movement is a critical stimulus to maintain tissue health. This is the “use it or lose it” principle we are all familiar with. This is important for the intervertebral discs and joint cartilage which have no direct blood supply and receive critical nutrition and metabolites though joint movement and imbibition. But movement is also critical for soft tissue like tendons, ligaments, and joint capsules.
This gets a bit complicated (in other words quite tedious and boring) so we’ll save the details for another time. Just know that through the process of mechanotransduction these tissues are able to sense movement and convert mechanical stimuli such as stretch and compression into important chemical signals. This signalling dictates the structure and function of the cell by controlling critical functions such as protein synthesis, gene expression, and calcium influx through stretch-activated membrane channels.
But mechanotransduction is not a systemic response. It’s not like aerobic exercise where the heart is similarly stimulated with cycling, running, swimming, or rowing. The individual cells are only stimulated when they directly receive a mechanical stimulus. In other words, if the spinal joints aren’t regularly stressed and don’t regularly move through a full ROM the cells are deprived of critical signalling needed to maintain tissue health. If this continues for any extended length of time the tissue starts to break down. A process known as immobilization degeneration.
So training isometrically may strengthen the muscles, but without moving the spinal joints through a full ROM there will only be a limited group of cells that experience the load and stress. It’s like making a sandwich but only putting the peanut butter on a tiny part of the bread. It’s not that it’s bad. But it’s incomplete
Traditional Stretching Isn’t Enough
So joint movement is critical. Here some may suggest that stretching the lower spine is helpful to get this movement stimulus to the spine. But just as I suggested that traditional “core” exercises were not the best way to train the spine, I would also suggest there are several shortcomings of traditional lower back stretches.
Remember the back is composed of a series of individual joints that form a moveable column. To be most effective we need to move and target these individual joints as much as possible.
But traditional stretches don’t do this. Think of a knee-to-chest or spinal rotation stretch, or common yoga movements such as cat-camel or child’s pose. All of these may create spine motion but none attempt to create focused or deliberate motion at the individual joints of the lumbar spine.
If I bend forward to touch my toes, or if I pull my knee towards my chest in an attempt to flex the lower spine which joints are flexing? The fact is we don’t really know. This is a major limitation of these traditional stretches.

And because the spine is a series of moveable segments it has an incredible ability to compensate for restricted joints. I don’t necessarily think these compensations are bad (we talked about this amazing ability of the body to compensate in our article on Rethinking Faulty Movement Patterns). But if the goal is to promote optimal movement and maximize health of the lower back I don’t think these types of traditional stretches are going to cut it.
We need better options. And that is where we need to turn to next.
Focus on Pelvic Tilts – The Key Movement for Spine
To be clear, it’s not that these traditional stretches or exercises discussed above are necessarily bad. I just think that for most back pain patients they aren’t the best options.
To be most effective, I think the movements and exercises need to fulfill certain criteria as outlined above. This is where pelvic tilts come in.
Pelvic Tilts for Focused Lumbar Motion
Now I know what you’re thinking. You’ve seen pelvic tilts before. But you haven’t seen them like this. The motions we’re going to talk about are not your typical pelvic tilts or basic cat-camel exercises.
The exercises that we’re going to review here allow us to check all the boxes. When done correctly they (1) create targeted and focused movement directly at the lumbar spine; (2) train the spine in a wide range of postures and positions (we can actually use these pelvic tilt based exercises to train the lower back in virtually any position possible – more on that in Part 3); and (3) provide a effective control stimulus for the nervous system.
Oh, and they can also be graded to match the needs of individual patients.
For example, in Part 2 we’ll discuss prescription options for acute low back pain and for patients who are sensitive to almost any form of movement or exercise. In Part 3 we’ll review exercises with a specific mobility and control focus. Here we will not only review how to promote more motion for tight and restricted spinal joints, but we’ll also discuss how to really home in on critical execution elements to build optimal joint control and coordination. Following that we’ll even review how to utilize these movements with a strength and endurance focus that will be challenging even for those with the strongest “cores”.
But first we need to review the basic movements themselves to provide context for the specific exercise prescriptions to follow.
Pelvic Tilts with a Flexion-Extension Bias
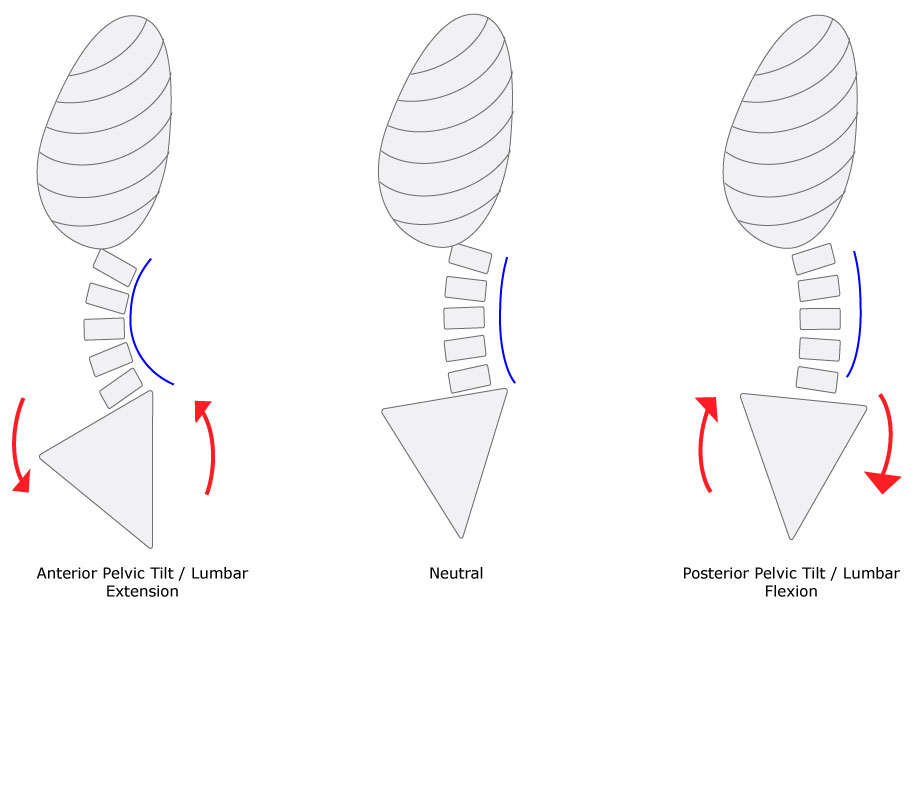
Remember the spine is a moveable column of block-like bones that sit atop one another. And this column sits atop the sacuum. So we can think of the sacrum and pelvis as the base or support platform of the spine. As a result, where the pelvis moves so goes the lumbar spine.
So as the sacral base rotates back during a posterior pelvic tilt the lumbar joints flex. This will create stretch and tension through the posterior aspect of the disc, joint capsules, and spinal ligaments. (Remember mechanotransduction – this stretch and motion is a powerful stimulus for tissue health and to maintain joint function).
Likewise, an anterior pelvic tilt will create motion in the opposite direction. This will help build and maintain lumbar extension. When done properly we can isolate the movement effect to the individual joints and muscles of the lumbar spine itself. And that’s the key.
And because these are active movements it creates a control challenge for the nervous system. It trains the CNS to better control lumbar motion. (How the motion occurs and the patterns of muscle contraction is critical here. We’ll talk about that in Part 3).
Pelvic Tilts with a Lateral Flexion / Rotation Bias
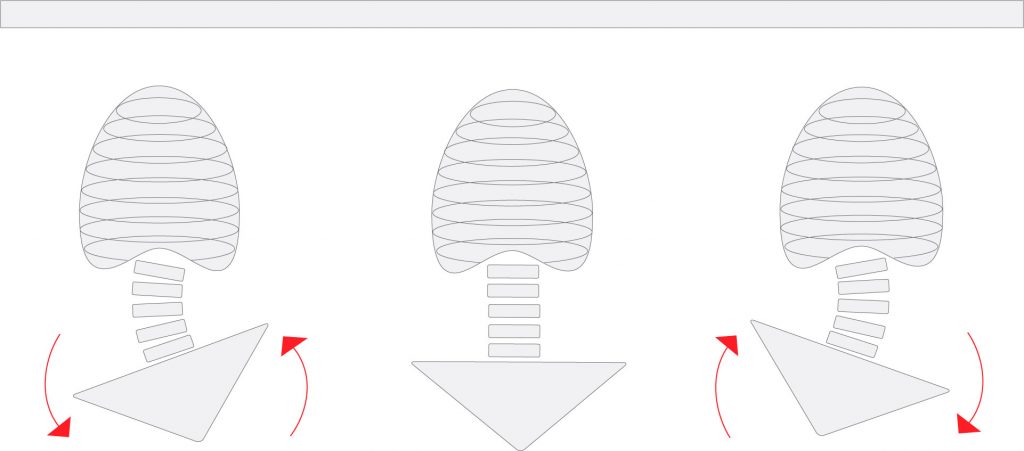
Traditional pelvic tilts are performed in the sagittal plane to create flexion-extension motion. But they can be performed in the frontal plane as well. This will create intersegmental lateral flexion (and because of coupled motion rotation as well) through the lumbar spine.
Lateral flexion to the right will open and create stretch and tension though the disc, joint capsules, spinal ligaments and deep intersegmental muscles on the left aspect of the spine. And again, because the motion is active it creates a control challenge and trains the CNS to better control the motion.
Next Steps….
So these are the critical movements. They form the foundation of virtually all of my lower back pain treatment programs. But as noted above this isn’t/ a one size fits all solution. Just doing these exercises isn’t going to magically fix back back pain.
These exercises need to be tailored to each individual patient. Both in terms of the movements themselves, but also with respect to programming (frequency, duration, intensity, etc).
That’s where we’ll turn next. In Part 2 we’ll talk about how to prescribe these pelvic tilt based exercises for patients in acute pain or for those patients who are sensitive to virtually any type of stretching or exercises.